When you think of “Amazon deforestation,” you probably think of the cute animals that are losing their homes to gold miners and farmers that are stripping the land. What you don’t tend to think of are the not-so-cute infections diseases that can spread from the drastic and devastating ecological changes caused by the deforestation. The reemergence of infectious diseases caused by deforestation has become a main concern of both epidemiologists and ecologists.
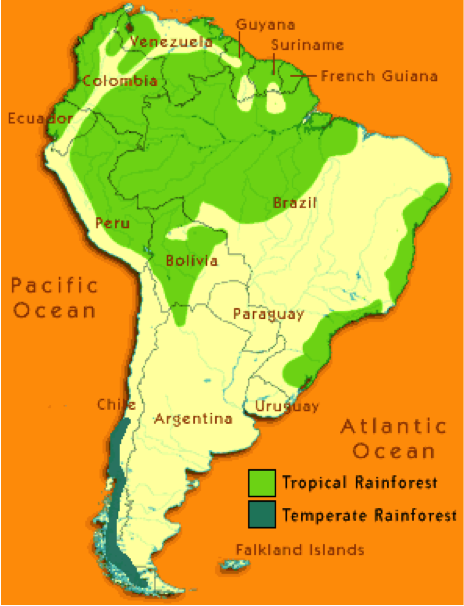
The current “problem child” of the diseases is malaria. In Peru, malaria eradication efforts of the 1960s dramatically decreased the prevalence of malaria in the northeastern region. This region is the part of Peru that contains the Peruvian Amazon Rainforest (Fig. 1). Up until the 1990s, this eradication effort remained successful at keeping the number of malaria cases at around 2.1 per 1,000 people. However, in 1997, the number of malaria cases jumped to 343 per 1000 people (Fig. 3). 154 of these 343 cases were caused by the parasite Plasmodium falciparum. Between the years 1983 and 1995, the rate of deforestation was at 4,257 hectares per year (Fig.2). The timing of the rise in deforestation and the rise in malaria cases had scientists wondering if deforestation was to blame for this increase in number of cases of a disease most everyone thought was history, and, if yes, why.
 |
|
Figure
1. Amazon Rainforest.
http://passporttoknowledge.com/rainforest/GEOsystem/Maps/s_america.html
|
 |
|
Figure 2.
Deforestation in Peru.
http://sp10.conservation.org/how/science/pages/deforestation-guides-for-commodity-sourcing.aspx
|
 |
|
Figure
3. Malaria in Peru.
http://www.cdc.gov/travel-static/yellowbook/2014/map_3-38.pdf
|
To answer these important questions, scientists first gathered data on how the biting rates of Anopheles darlingi, a mosquito that is most efficient vector of malaria in the Amazon Basin+, changed depending on the amount of deforestation at the location of study. A study was conducted by Amy Yomiko Vittor et. al. that examined the location of A. darlingi to try and produce concrete evidence that areas with more deforestation held a higher population density of A. darlingi. They set up studies in 14 human-altered sites (meaning sites with deforestation) and 5 unaltered sites. They found A. darlingi in 13 out of the 14 altered sites, and none was found in the unaltered sites, suggesting that certain human activities that clear a large amount of forest (i.e. gold mining, cattle ranching and logging) increase malaria risk (Fig. 4). This study, however, only assessed the risk associated with more A. darlingi (more mosquitoes equals more possible malaria carriers). It did not produce data on the number of A. darlingi that were infected with the malaria parasite.
 |
|
Figure 4. Amy Yomiko Vittor et. al. Impact of Deforestation on Malaria Risk. Am. J. Trop. Med. Hyg., 74(1) 4 (2006). |
Now the question to be answered was why were there more A. darlingi in deforested areas than in unaltered areas? Knowing mosquito larvae grow in shallow stagnant water pools, Amy Yomiko Vittor et. al. figured out that the reason why deforested areas contained more A. darlingi was because these areas had more possible breeding grounds for them than unaltered areas. Deforested areas contain many stagnant water pools, as well as fish farms, which are other favorite spots of A. darling.
Even though this study was conducted in the late 90s and early 2000s, the problem is still prevalent today. Scientists have proposed several solutions that could help reduce deforestation, which would reduce the number of A. darlingi present and reduce malaria risk as a whole. The first proposed solution is to regulate more closely agricultural practices. This regulation could help reduce the number of stagnant water pools in farms, limiting the places A. darlingi would be able to reproduce. Another suggested solution is to have stricter laws on human settlement. Population growth leads to a higher demand for settlement land, which is often provided through the deforestation of the rainforest. Scientists are proposing that laws be put in place to ban completely stripping the land. The people would instead find natural clearings or only remove some of the vegetation.
So, you may be thinking “How does this affect me? I’m not going to Peru any time soon.” Well, the problem is that as the number of malaria cases rises, antimalarial drug use increases. Increased drug use can lead to resistance among the pathogens, and that resistance can spread. Scientists are already seeing strains of Plasmodium falciparum emerging that are immune to the most commonly prescribed antimalarial drug Chloroquine. Luckily, Plasmodium falciparum is a parasite, so it cannot share resistant genes like bacteria can. Resistance occurs when there is a mutation in the parasite’s genes, so resistance can only be passed to offspring. The problem then becomes that the antimalarial drug kills off nonresistant parasites, leaving an environment for the resistant ones to thrive. However, malaria treatment prospects show that combinations of drugs can be used to kill both the resistant and nonresistant parasites.
+A vector is an organism that carries a pathogen and transmits it to another living organism. In this case, A. darlingi was carrying Plasmodium falciparum. It is considered the most effective vector because it carries malaria parasite in its salivary glands and most often feeds on humans.
References:
Amy Yomiko Vittor et. al. "The Effect Of Deforestation On The Human-Biting Rate Of Anopheles Darlingi, The Primary Vector Of Falciparum Malaria In The Peruvian Amazon" in The American Society of Tropical Medicine and Hygiene, 74(1), 3–11 (2006).
Amy Y. Vittor et. at. "Linking Deforestation to Malaria in the Amazon: Characterization of the Breeding Habitat of the Principal Malaria Vector, Anopheles darling" in The American Society of Tropical Medicine and Hygiene, 81(1), 5–12 (2009).
White, Nicholas J. "Antimalarial Drug Resistance" in J. Clin. Invest. 113(8), 1084–1092 (2004).
Yasuoka, Junko and Richard Levins. "Impact Of Deforestation And Agricultural Development On Anopheline Ecology And Malaria Epidemiology" in The American Society of Tropical Medicine and Hygiene, 76(3), 450–460 (2007).
You mentioned in your blog that individuals living in developed countries should be aware of malaria due to the possible resistance the parasitic virus can develop towards drugs; however, I feel as though malaria is a bigger threat than that. Since malaria is a vector-based parasitic virus, it can be carried and transferred much faster than transmission through human-to-human contact. Within the U.S., we face the threat of the West Nile Virus which is also a vector-based virus. Therefore, I believe the threat of emerging infectious should not just be targeted at the malaria in developing countries, but any country with harmful vector-based viruses.
ReplyDeleteYou mentioned in your blog that individuals living in developed countries should be aware of malaria due to the possible resistance the parasitic virus can develop towards drugs; however, I feel as though malaria is a bigger threat than that. Since malaria is a vector-based parasitic virus, it can be carried and transferred much faster than transmission through human-to-human contact. Within the U.S., we face the threat of the West Nile Virus which is also a vector-based virus. Therefore, I believe the threat of emerging infectious should not just be targeted at the malaria in developing countries, but any country with harmful vector-based viruses.
ReplyDeleteThe climate and location does make total sense for the high number of cases of Malaria, but it is unfortuante that such a disease occurs in a third world area and if it were to happen in America for example, the treatments and cures would be readily availible.
ReplyDeleteAs humans, we often underestimate the benefits we get from the environment. Many consider deforestation and other environmental destruction justified in the name of industrial progress, but it's times like this when we realize that our actions can facilitate a cascading effect and have a far larger impact than expected. Now that we are seeing public health complications, I wonder how these will influence ongoing conservation effort and policy in the years to come.
ReplyDeleteVery interesting post, I think it is important to understand the impacts we have on the world around us. For a while people did seem to have the attitude of oh well, it doesn't affect me so why should I care? Now we are starting to really see that all of our actions have consequences, and that the best way of dealing with these consequences seems to be prevention. I agree with Sarah, we need to replenish these depleted forests before this becomes a problem for us, not after.
ReplyDelete